
Experiencing abdominal discomfort can be unsettling, especially when its origin is uncertain. Appendicitis and ovarian cysts are potential sources of abdominal pain, each presenting distinct symptoms and…

Experiencing abdominal discomfort can be unsettling, especially when its origin is uncertain. Appendicitis and ovarian cysts are potential sources of abdominal pain, each presenting distinct symptoms and…

Urinary tract infections (UTIs) can be uncomfortable and, in some instances, escalate to serious health concerns. While numerous UTIs can be managed using at-home remedies and over-the-counter…
When it comes to maintaining our overall well-being, few things are as fundamental as proper hydration. Our bodies are predominantly composed of water, with approximately 60%…

When it comes to managing type-2 diabetes, Ozempic has emerged as a valuable tool. This FDA-approved medication offers hope to countless individuals seeking to regulate blood sugar…

Vomiting is a common symptom that can be caused by various factors, from mild stomach bugs to more serious underlying conditions. Understanding when to seek emergency…
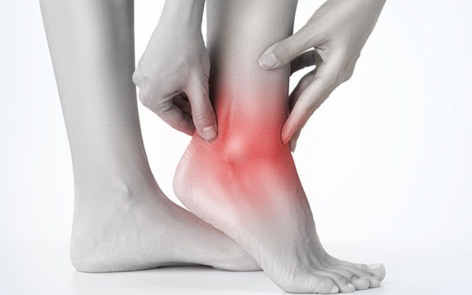
Ankle pain that shoots up your leg can be debilitating and concerning. Understanding the causes, treatment options, and recovery process is crucial for anyone experiencing this discomfort.…
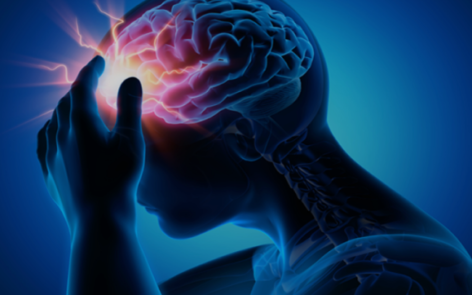
Suffering a concussion can be a distressing experience, but knowing what to expect when you seek help at the Emergency Room (ER) can provide clarity during…

Embarking on a detox journey can be enticing, promising to flush out toxins and boost your overall well-being. However, beneath the allure of detoxification lies a potential…

Iron deficiency anemia is a prevalent condition that arises when your body lacks sufficient iron to produce an ample number of healthy red blood cells. While many…

Fever, a common symptom across various illnesses, often brings discomfort and raises questions about when it warrants a trip to the Emergency Room (ER). While many fevers…

Thomas Hintz is a Senior Editor, focusing on clinical informatics, learning health systems and value-based care transformation.
By Thomas Hintz
By Thomas Hintz
By Thomas Hintz
By Thomas Hintz

Find an answer to the question "What are my lucky days to gamble?" in the new Gambling Horoscope created by the CasinoHEX team. Discover lucky gambling days for Libra, Virgo, Cancer, Gemini and the rest of the zodiac signs. Find a perfect online casino and make your lucky bet!

Fresh 2021 No Deposit Casino Bonuses only on CasinosAnalyzer
Our project got a new partner from Poland - the PlayBison brand with the support of Milan Rabszski. We are starting a joint journey and look forward to productive cooperation in the future.

The Most Comprehensive Car Specs Database. Over 40.000 technical specs, dimensions, fuel consumption!

Are you looking the most profit online casino for Norwegian players? Maria casino is one of the best gambling platform to earn money and get fun!

Get live tennis scores, tennis news, tennis livescores & more at TennisBoard – the #1 tennis livescore website. Use comprehensive sports data, statistics and tables to improve prediction and odds valuation when sports betting.

This guide is for those looking to experience the top-rated online pokies at regulated Australian casino sites. With numerous online casinos offering real money pokies, it can be a daunting challenge to locate the ideal one.

Are you looking for real money casinos in Australia? Onlinecasinos-australia.net is a leading online gambling site for Aussie players.

Unleash the potential of radiant skin, strengthened hair, and healthier nails through the nourishing power of this exceptional biotin and collagen supplement.

BEST CASINO24 is a popular casino site of Woori Casino.